
Unveiling the Ethical Elegance of Lab-Created Diamonds
In the realm of fine jewelry, diamantes éticos de laboratorio or lab-created diamonds have emerged as a shining beacon of… Read more »
Prologue to Semaglutide Pill Semaglutide has arisen as a promising treatment choice for people battling with type 2 diabetes … Read more »
Introduction Teenage years can be tumultuous, with the rollercoaster of emotions the challenges that come with adolescence. One crucial… Read more »
Antioxidants: Silent Guardians of Our Health Lutein: Not Just for Eyes Anymore Building Immunity Through Smart Supplementation Exercise: Your Immune… Read more »
Are you tired of feeling fatigued, moody, lacking energy? Have you ever considered using testosterone therapy to help improve… Read more »
The world of healthcare is evolving, so is the way we access essential medications. Online Pharmacies Canada have emerged… Read more »
Mobility scooters play a vital role in enhancing the lives of individuals with limited mobility. For more on top outdoor… Read more »
When we think of self-care, we often think of taking care of our physical needs, such as getting enough sleep,… Read more »
Did you know that your body can absorb about 25 grams of protein in one sitting? Your body roughly takes… Read more »
The respiratory system is the set of organs tissues in your body that facilitate breathing. Using the oxygen in… Read more »
Two potent anabolic steroids that are frequently used in bodybuilding athletic performance enhancement are trenbolone acetate nrolone decanoate…. Read more »
Two potent anabolic steroids that are frequently used in bodybuilding athletic performance enhancement are trenbolone acetate nrolone decanoate…. Read more »
Even when you or a member of your family is ill, sting in line at the drugstore is not enjoyable,… Read more »
Dental pains are unpredictable extremely tormenting. If you are experiencing an extreme toothache or bleeding gum right in the… Read more »
If you’ve experienced a traumatic incident, you may be feeling the effects of post-traumatic stress disorder. PTSD is a serious… Read more »
Hygiene is not something you must do because others are doing, it is essential if you want to maintain good… Read more »
Numerous failed weight loss attempts can cause one to search for alternate methods to lose weight. The good news is… Read more »
Health insurance in India is generally confined to persons over the age of 40 who are at risk or suffering… Read more »
Botox is a household name is used for a wide variety of medical cosmetic treatments. There are millions… Read more »
Botox is a popular treatment for facial wrinkles that has been around since the 1980s. It is a neurotoxin that… Read more »
With nose augmentation surgery, you can get a more defined smoother nose. You can also get a more masculine… Read more »
Vitamin C is a type of water-soluble antioxidant that is very effective in fighting against free radicals. It is a… Read more »
To look younger more youthful, you need to make sure that you are taking care of your skin. A… Read more »
By golly, there certainly are a lot of different things in the world of medicine, aren’t there? More words than… Read more »
Most people will see the best orthopaedic at some point in their lives, some people will see them often…. Read more »
Teeth. We’ve all got ‘em. Well, most of us do. We could, at the very least, say that everyone has… Read more »
Afikim Electric Vehicles, also popularly known as Afiscooters, is among the most reputable heavy-duty mobility scooter manufacturers globally. They are… Read more »
Cosmetic injectables are game-changers for reaching your aesthetic goals. Both Botox dermal fillers can achieve beautiful results, whether you… Read more »
When it comes to pain management, there are a lot of solutions available. Some of these solutions may work better… Read more »
Zoom Complies with HIPAA Rules The most important concern for every society is suffering from mental health issues because… Read more »
A Pleasant Atmosphere Is One Thing To Look For Before you schedule an appointment at a medical spa, there are… Read more »
Support groups can work wonders for people that are currently diagnosed with cancer or recovering from it. There is a… Read more »
If you are a dog enthusiast, you might have come across the statement that CBD products can benefit a dog’s… Read more »
When it comes to the pros cons of the Athenahealth EHR, there are three major advantages that the company… Read more »
If you have decided to use Anabolic steroids for bulking up shred body fats, you need to follow the… Read more »
Going to rehab for addiction treatment seems like it’s the only option you have. While these programs can be beneficial,… Read more »
Though the average lifespan of Americans is 79 years, these numeric quantities do not really have quality in terms of… Read more »
Aronia berries are native to North America are believed to have positive effects on health, with previous studies suggesting… Read more »
Over the last few years, there has been a lot of buzz going around about terpenes. Since people have discovered… Read more »
If you have borderline personality disorder (BPD), it’s likely that you use alcohol or other drugs in an attempt to… Read more »
Adderall is a physician-endorsed drug a CNS energizer that is utilized to deal with the infections like narcolepsy … Read more »
Suppositories have a base made from substances such as cocoa butter or gelatin that surrounds the drug. As the warmth… Read more »
When you are searching for a reliable gynecologist in your area, you should start your research visit a gynecologist… Read more »
Cannabis is an important plant that comes with a myriad of benefits. However, it starts right from its seeds before… Read more »
The coronavirus pemic has caused many people to question their career professional decisions. It’s even been a challenging time… Read more »
Omega 3 fatty acids are an integral part of your diet. They are made up of both EPA (Eicosapentaenoic acid)… Read more »
If you know someone who is struggling with addiction, it is important that you help them out. You never know… Read more »
Marijuana is nowadays used for a variety of reasons, both medical recreational. Since many states have now legalized it,… Read more »
These days, cannabis edibles are so many that it can be challenging to select the best one for your… Read more »
Hair Transplant Surgery, also known as Hair Restoration Surgery, is a medical technique that restores hair to the bald areas… Read more »
People from all over the world, including a large part of the United States, absolutely love Avene products. This is… Read more »
Are you looking for the best way to prevent posture cancer? Do you need to extend your lifespan? Want to… Read more »
Marijuana dispensaries were fiction back in the days. For the individuals who needed weed products, there were only a few… Read more »
As states continue to legalize cannabis in the US, most people are becoming more interested in infusing this product in… Read more »
You probably are aware of dental cavities, tooth decay, related tooth problems. And that sugar feeds the bacteria that… Read more »
Are you tired of getting painful UTIs? Get ready to Kiss That UTI Goodbye with the long-awaited urinary tract support… Read more »
Gastritis is the condition in which the protective lining of the stomach becomes inflamed. People can have both acute … Read more »
When you start taking drugs or any addictions in your life, it is needed to eliminate the addiction as… Read more »
More than sixty percent of an adult’s body constitutes water. Water is vital to life. A body might not function… Read more »
Chlamydia Symptoms Testing. Chlamydia is a STD (sexually transmitted disease) caused by a virus called the Human Papilloma Virus… Read more »
Typically, rehabilitation centers for people last about twenty-eight days to ninety days long. But this period isn’t enough for one… Read more »
The face is a reflector of our feelings so everyone wants to get a fresh youthful-looking face. As non-surgical… Read more »
Here are ways that you could bring up STD test awareness to your doctor or nurse: * Have ever been… Read more »
Finding out that you have Parkinson’s Disease (PD) is a life-changing development. Everyone receives this news differently, with most people… Read more »
Injury in the knee can cause severe pain discomfort. Knee surgery is the best way to get rid of… Read more »
Day by day there remain various characters do craving to visit Mumbai for getting drug rehabilitation treatment. The Drug Rehabilitation Centre… Read more »
Rationale directs it’s ideal to have cbd oil with melatonin just before sleep time cbd for energy a couple… Read more »
If you are feeling stressed depressed, then you need to find the root cause of the problem work… Read more »
There are days when you lack motivation for workouts need that extra push. Pre workout pills provide that push… Read more »
Cosmetic dentistry is one of the greatest cosmetic procedures completed in the cosmetic market. Folks want lovely smiles. They might… Read more »
Are you a workout enthusiast? You love spending time in the field. It is an amazing moment lifting weights. Also,… Read more »
In order to start existence over within positive methods drug rehab is the solution. You deserve to reside a existence… Read more »
Who do we consider when we hear the word psychotherapist? A maintained clinical social expert exists in the field of… Read more »
Eight out of ten people do not fully underst what physiotherapy is all about. It is no wonder; after all,… Read more »
Deciding to seek treatment for substance abuse is a crucial first step in your recovery process. You’ve immediately accepted that… Read more »
On the off chance that you are among the individuals who have come to think about CBD oil, hemp blossom… Read more »
Cannabinoids are one of the compounds which make up cannabis. Research has proved that more than 100 cannabinoids are found… Read more »
The stresses of everyday life are intense to say the least. Some of us find them too much to bear,… Read more »
Planets are really active forces in determining your health conditions. It’s better if you know prior what type of body… Read more »

In the realm of fine jewelry, diamantes éticos de laboratorio or lab-created diamonds have emerged as a shining beacon of… Read more »

At Lab Diamonds Are The Future, we pride ourselves on being at the forefront of innovation in the world of… Read more »

In the realm of diamonds, size isn’t just a matter of glamour; it’s a reflection of beauty, brilliance, sophistication…. Read more »

In the realm of eternal love commitment, the choice of an engagement or wedding ring holds profound significance. As… Read more »

When it comes to purchasing a ring, whether it’s for a special occasion or a daily accessory, getting the right… Read more »

At our company, we underst the allure of diamonds—their timeless beauty, their captivating sparkle, their symbolic significance. However, in… Read more »

Prologue to Semaglutide Pill Semaglutide has arisen as a promising treatment choice for people battling with type 2 diabetes … Read more »

Introduction: Sparkling Surprises Await Have you ever wondered about the stories hidden within the glimmer of a diamond ring? What… Read more »
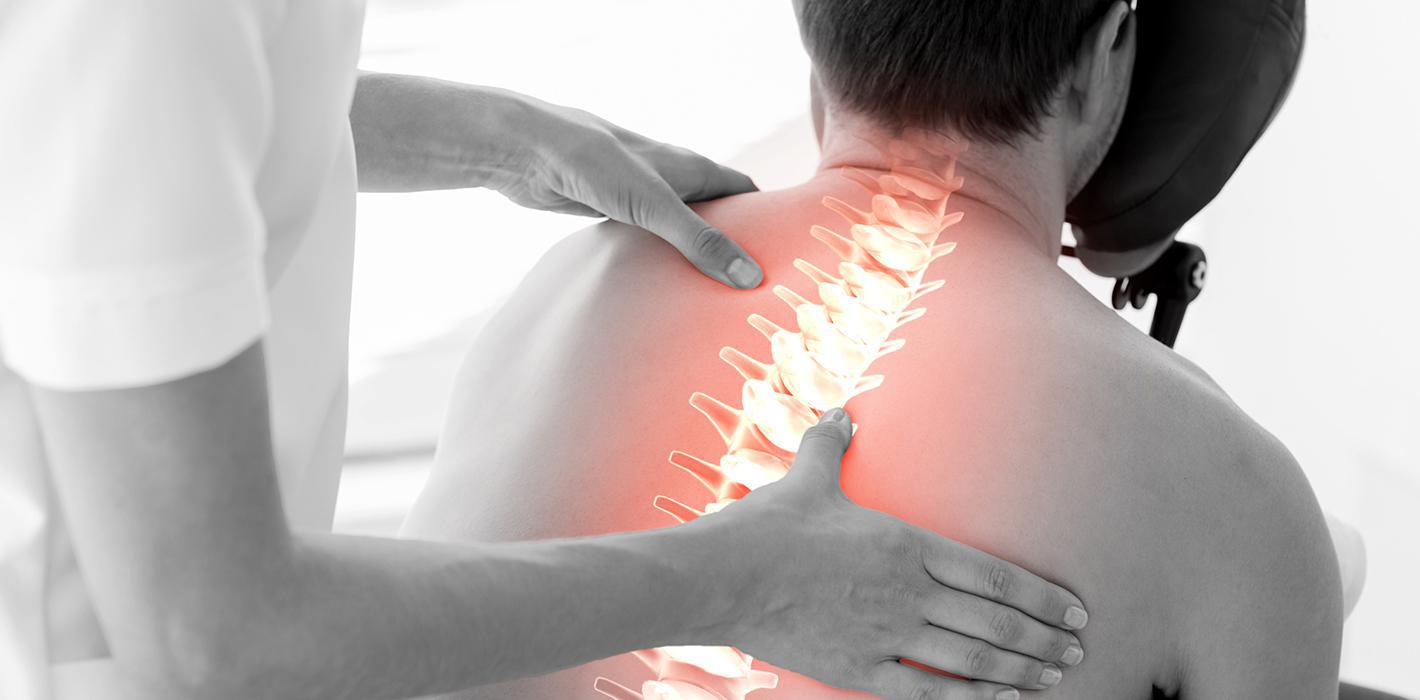
Are you satisfied with your current body mass index (BMI)? Do you feel that it might be time to shed… Read more »

Introduction Teenage years can be tumultuous, with the rollercoaster of emotions the challenges that come with adolescence. One crucial… Read more »
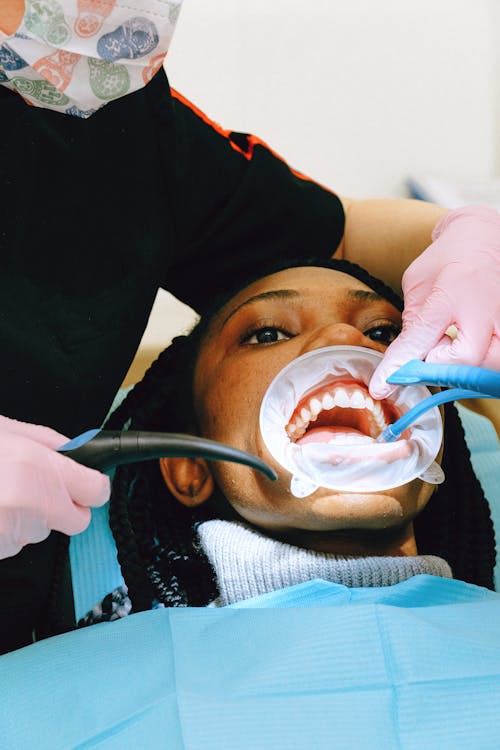
A smile can speak volumes, but unexpected dental mishaps can lead to distress when that smile includes dentures. Denture emergencies… Read more »

In today’s fast-paced corporate world, fostering a sense of camaraderie among team members is crucial for productivity overall success…. Read more »